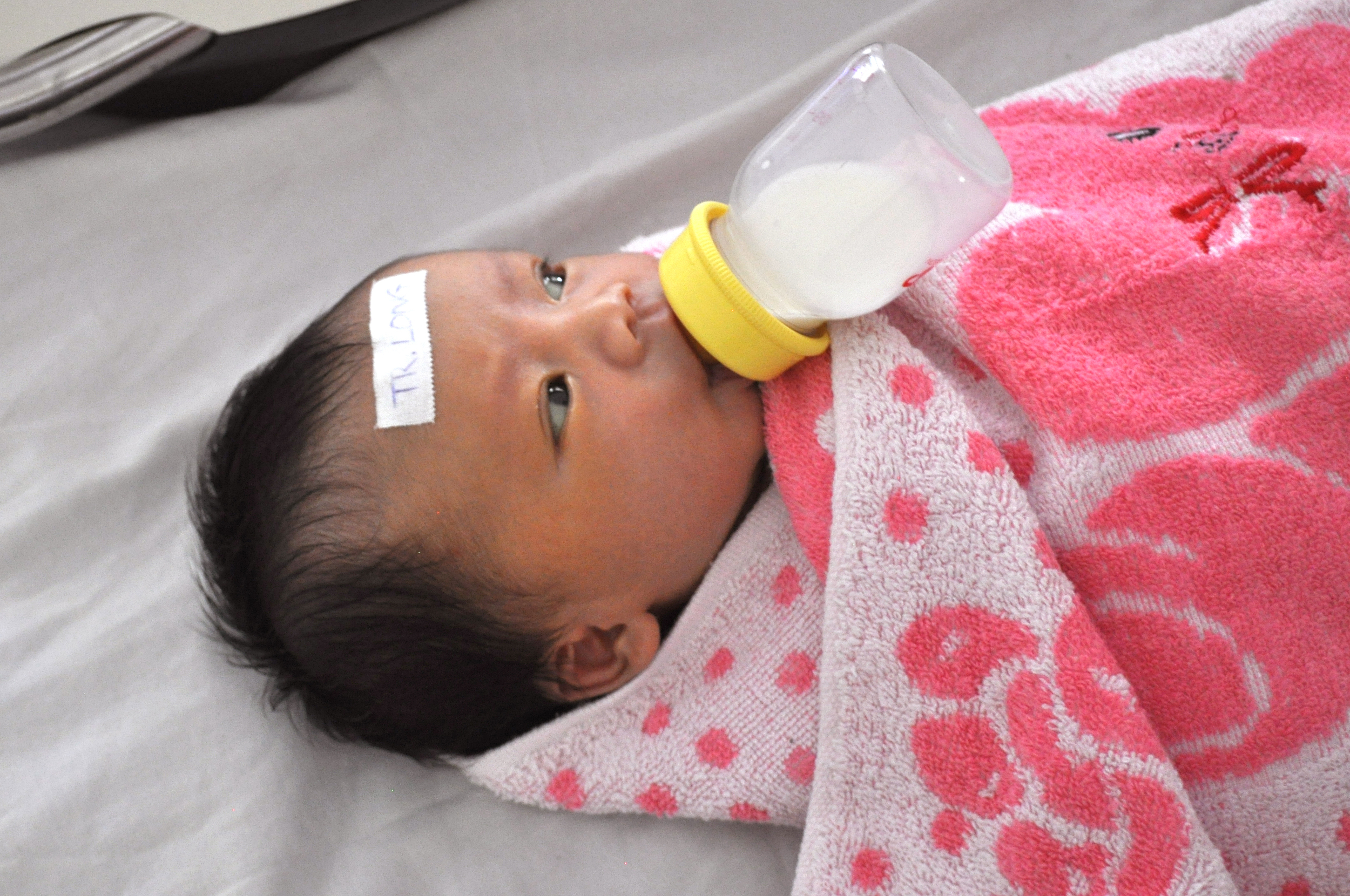
A recently published study (Arnolda et al., BMC Pediatrics, 2015) demonstrates the impact of high-intensity phototherapy in averting the need for costly and dangerous exchange transfusions among at-risk newborn patients in low-resource settings.
Exchange transfusions are a treatment of last resort for severe jaundice. In the procedure, the newborn’s blood is slowly withdrawn via catheter and fresh, prewarmed blood or plasma is pumped into the newborn's body. This cycle is repeated, resulting in a removal of about 90% of the original blood cells and about half of the vascular bilirubin. The procedure is particularly challenging in low resource countries, where the donor blood supply is limited and there is a higher prevalence of transfusion-transmissible infections.
Phototherapy has been proven by randomised trial to markedly reduce the need for exchange transfusion in high resource settings (Brown et al, Pediatrics, 1985), so the Arnolda study sought to quantify the reduction possible in a low resource setting. Conducted at four hospitals in Myanmar, the study confirmed that compared to conventional, low-intensity phototherapy, high-intensity LED phototherapy can result in a 33% reduction in exchange transfusions among transfer patients (neonates born outside the medical care center).
An earlier study (Arnolda et al, Maternal Health, Neonatology and Perinatology, 2015) validated DtM partner Thrive Networks’ experience with high incidence of severe newborn jaundice in Myanmar and many other countries. Another recent paper (Olusanya et al., Archives of Disease In Childhood, 2014) explains why delays in the diagnosis of jaundice and the start of treatment are common in developing countries, and how as a consequence these settings experience a much higher incidence of severe jaundice than industrialized countries.
These research findings represent an important validation of the value proposition for DtM’s Firefly Phototherapy Device. At the time of diagnosis in developing countries, jaundice presents almost as a different and more severe disease. Given the limited resources in these countries (everything from unreliable power supplies to lower staff-to-patient ratios), it’s unlikely that a phototherapy device designed for US or EU conditions will be appropriate for long-term use in low-resource settings. It’s hard to imagine how there could be a single “one size fits all” or “world class” standard for even a relatively simple medical technology like phototherapy.
Firefly provides high-intensity phototherapy from above and below the newborn, covering a significantly larger skin surface area than single-sided devices designed to the international standard. Fixing the position of the lights with respect to the bassinet also eliminates opportunity to user error that might occur in settings with limited user training and a much greater number of patients per caregiver. These features allow Firefly to treat neonates who might otherwise require an exchange blood transfusion.