Otter Newborn Warmer
A conductive warmer for preventing and treating newborn hypothermia in low-resource settings.
About
Otter is a newborn conductive warmer designed specifically to prevent and treat newborn hypothermia in low-income countries among admitted patients and during in-hospital transportation, for users with limited training in areas of electricity insecurity.
Unlike the incubators and radiant warmers a rural hospital might receive as donations or through a government purchase, the Otter Warmer provides effective newborn warming that is “hard to use wrong”. Otter features an intuitive touchscreen interface, seamless polycarbonate construction for infection control, and integrated battery providing uninterrupted warming during power failures.
Otter received Vietnam and ASEAN regulatory approval as a Class B device in March 2025, and CE Mark under the European Medical Device Regulation 2017/745 (EU MDR) in January 2026.
Keeping Newborns Warm
Medical devices designed for high-income countries often prove unsuitable for hospitals in low- and middle-income countries. International standards for medical devices assume ideal clinical conditions–including reliable infrastructure, resources and staff capabilities–that are uncommon in low-resource settings, particularly in public care facilities.
Otter differentiates itself in a market dominated by expensive, complex solutions. International standards prioritize efficacy (ideal conditions) over effectiveness (real-world conditions). Traditional incubators and radiant warmers are expensive, maintenance-intensive, and require stable power, making them unsuitable for rural hospitals in poor countries.
Otter applies three principles: context-appropriate (adapting to electricity insecurity), appears effective (quality aesthetics signal trustworthiness to overloaded staff), user-friendly (eliminating "latent errors").
Otter resembles a standard newborn bassinet, which helps mothers overcome worries about interacting with a complex medical device, and facilitates mother-child bonding.
The Global Burden of Newborn Hypothermia
Neonatal hypothermia is defined as the state in which a newborn’s body temperature drops below 36.5°C. Hypothermia is recognized as a comorbidity factor to the three main direct causes of neonatal death: preterm birth, severe infection, and asphyxia [1]. Preterm birth is responsible for 60% to 80% of all newborn deaths, and preterm babies are at a higher risk for developing hypothermia. Preterm babies require immediate and continuous warming in order to survive.
A high prevalence of hypothermia is reported from countries with the highest burden of neonatal mortality [2], even in warmer tropical environments [3].
Clinical experts and field staff identified three stages in the newborn treatment journey with higher incidence of newborn hypothermia: transport to and within clinical facilities, during admission processing and during hospital stays in the newborn unit [4].
Although KMC is effective, studies show that even a 30-minute break in warming can result in the onset of neonatal hypothermia [5]. Even in settings with good KMC compliance, breaks in warming are unavoidable, for example when the mother needs to wash or go to the toilet, or when the newborn becomes too unstable for KMC. Supplemental warming is necessary to avoid newborn hypothermia.
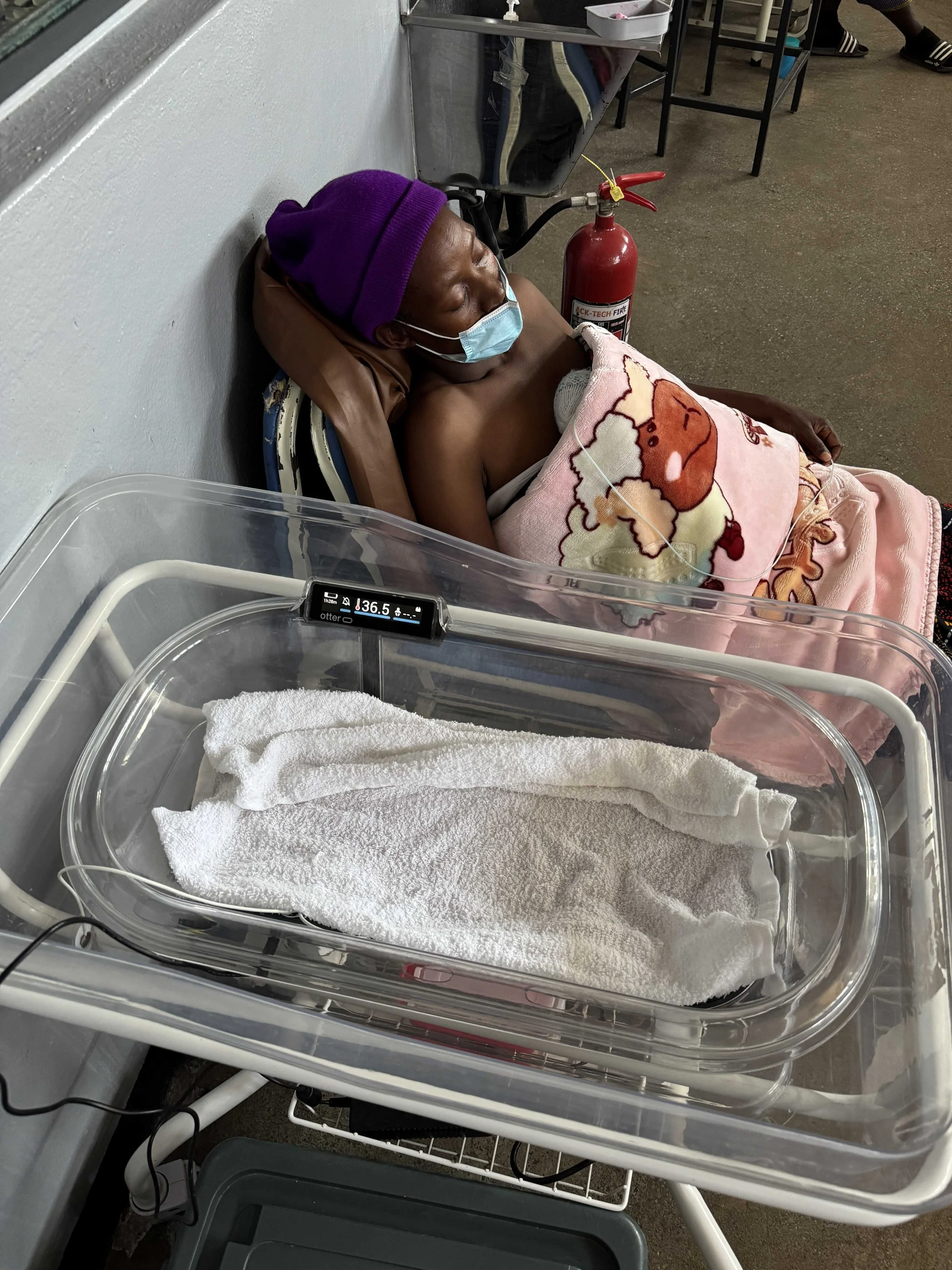
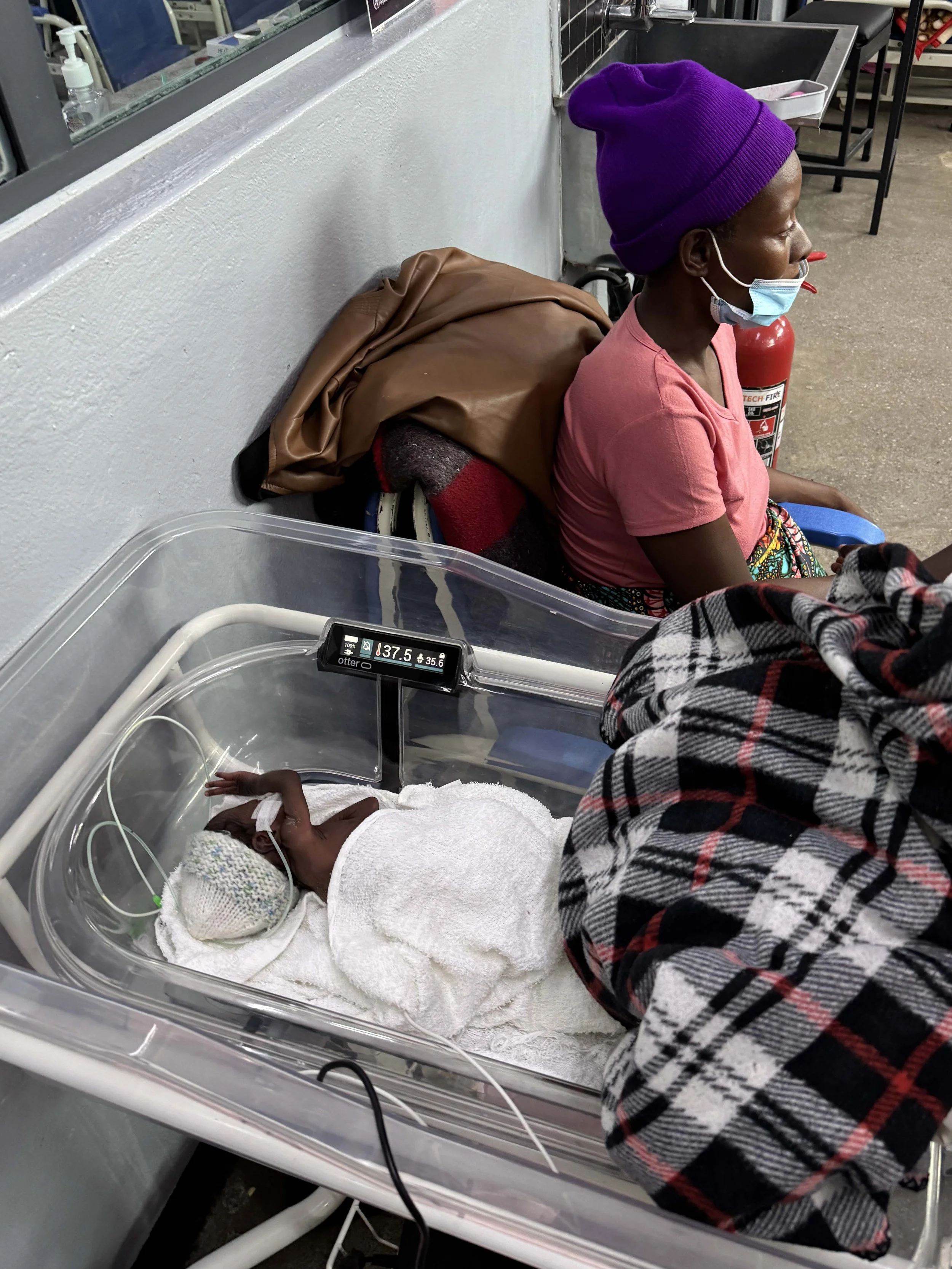
A premature newborn weighing 1,050g receiving kangaroo mother care (KMC) at Kapiri Mposhi District Hospital in Zambia
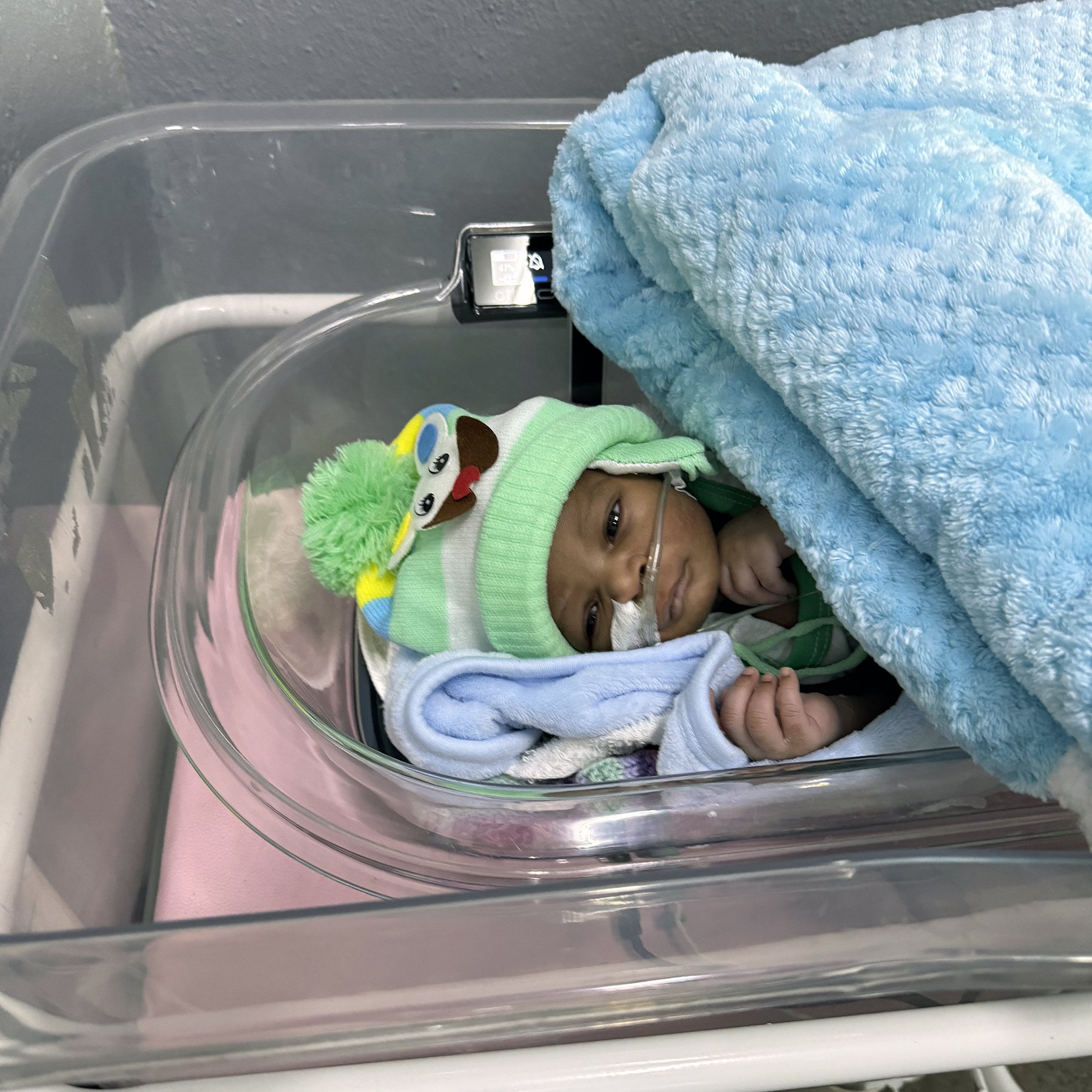
Otter providing supplemental warming to the same newborn while the mother takes a break from skin-to-skin care.
[1] K. Lunze, D. E. Bloom, D. T. Jamison, and D. H. Hamer, “The global burden of neonatal hypothermia: Systematic review of a major challenge for newborn survival,” BMC Medicine, vol. 11, no. 1, p. 24, Dec. 2013, ISSN: 1741-7015. DOI: 10.1186/1741-7015-11-24.
[2] R. Onalo, “Neonatal hypothermia in sub-Saharan Africa: A review,” Nigerian Journal of Clinical Practice, vol. 16, no. 2, p. 129, 2013, ISSN: 1119-3077. DOI: 10.4103/1119-3077.110120.
[3] M. Saaka, F. Ali, and F. Vuu, “Prevalence and determinants of essential newborn care practices in the Lawra District of Ghana,” BMC Pediatrics, vol. 18, no. 1, p. 173, May 2018, ISSN: 1471-2431. DOI: 10.1186/s12887-018-1145-4.
[4] T. Prestero, S. Janet, M. Kyokan, et al., “Neonatal Hypothermia: A Solution-Focused Field Assessment in Bangladesh,” MSF Paediatric Days 2021 - Virtual Edition, 2021. DOI: 10.13140/RG.2.2.11252.27529.
[5] S. Rao, P. Thankachan, B. Amrutur, M. Washington, and P. K. Mony, “Continuous, real-time monitoring of neonatal position and temperature during Kanga- roo Mother Care using a wearable sensor: A techno-feasibility pilot study,” Pilot and Feasibility Studies, vol. 4, p. 99, 2018, ISSN: 2055-5784. DOI: 10.1186/ s40814-018-0293-5.
About Conductive Warming
Studies conducted over the past 30 years conclude that conductive warming is a non-inferior method for preventing and treating hypothermia compared to other standards of care [1]. In some cases, the conductive warming mattresses were more effective than incubators at helping newborns reach and maintain a stable temperature [2]. A literature survey performed in 2017 of fifteen different trials concluded that conductive warming is a safe and effective method for treating and preventing hypothermia [3].
[1] C. Green-Abate, N. Tafari, M. R. Rao, K. F. Yu, and J. D. Clemens, “Comparison of Heated Water-Filled Mattress and Space-Heated Room with Infant Incubator in Providing Warmth to Low Birthweight Newborns,” International Journal of Epidemiology, vol. 23, no. 6, pp. 1226–1233, 1994, ISSN: 0300-5771, 1464-3685. DOI: 10.1093/ije/23.6.1226.
[2] I. Sarman, G. Can, and R. Tunell, “Rewarming preterm infants on a heated, water filled mattress.,” Archives of Disease in Childhood, vol. 64, no. 5, pp. 687–692, May 1989, ISSN: 0003-9888, 1468-2044. DOI: 10.1136/adc.64.5.687.
[3] J.-P. Libert, S. Delanaud, and V. Bach, “Warming mattresses for newborns: Effectiveness and risks,” Biomedical Journal of Scientific and Technical Research, vol. 1, no. 7, pp. 001–004, Dec. 2017. DOI: 10.26717/BJSTR.2017.01. 000608.
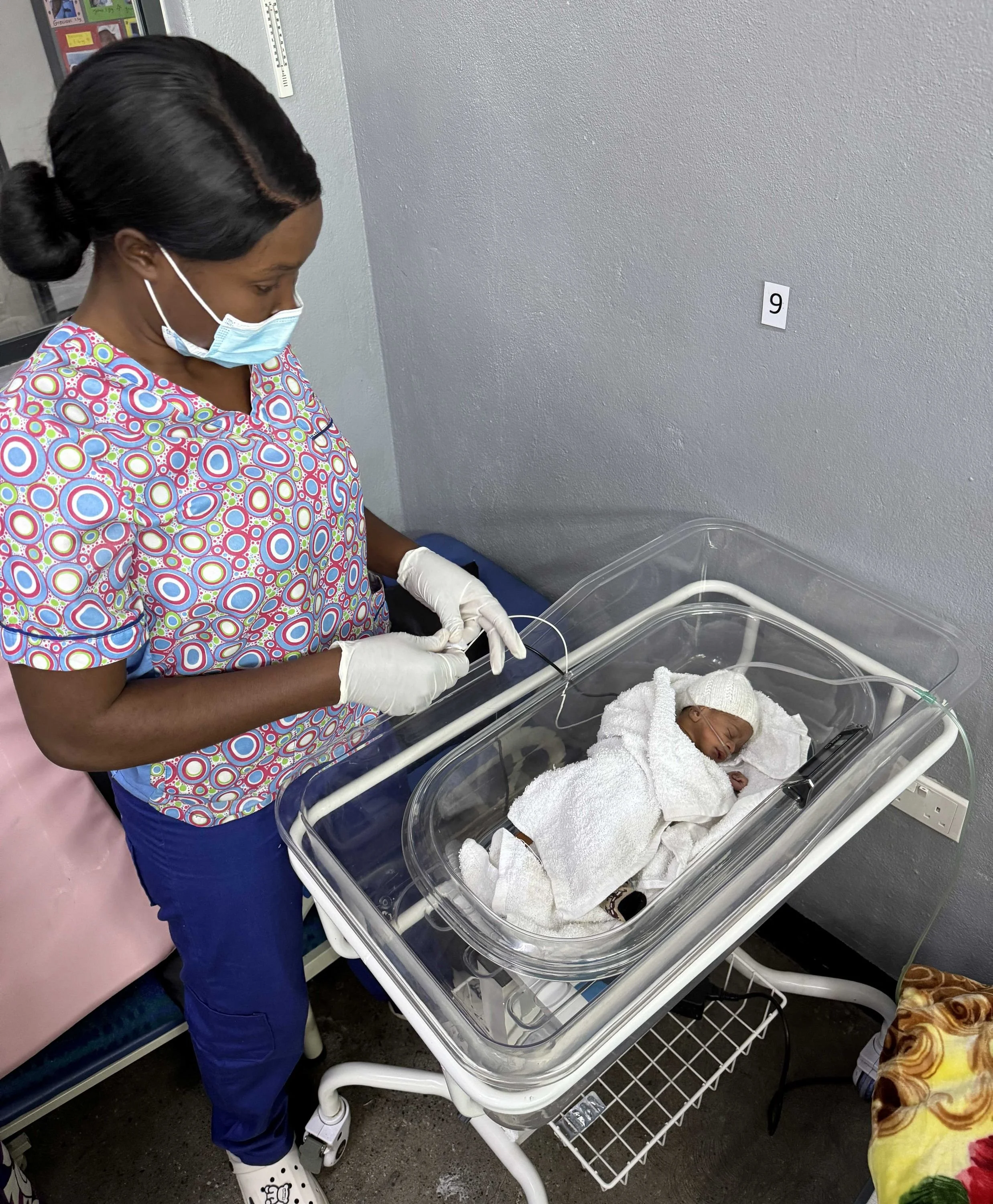
Clinical staff resuscitating an unstable 1,600g newborn inside Otter at Kapiri Mposhi District Hospital in Zambia
The Otter bassinet has a smooth internal surface with no fabric, seams or gaps, and can be quickly disinfected with standard hospital cleaning products.
Infection Prevention and Control
Nosocomial or hospital-acquired infections are one of the leading causes of mortality and morbidity in neonatal intensive care units [1]. A 2009 study found that despite national guidelines requiring frequent and thorough cleaning and disinfection of newborn health equipment, bacteria were isolated from 35% of incubators in a Cairo newborn unit [2]. Compared to a soft mattress, a seamless firm surface is easier to properly clean and disinfect between patients.
[1] Gray, J., and N. Omar. “Nosocomial Infections in Neonatal Intensive Care Units in Developed and Developing Countries: How Can We Narrow the Gap?” Journal of Hospital Infection 83, no. 3 (2013): 193–95. DOI: 10.1016/j.jhin.2012.12.006.
[2] Abd El Haleim, Mona M, Nada N Nawar, and Eman M Abd El Rahman. “Epidemiologic and Microbacteriologic Study of Neonatal Septicaemia in Cairo University Neonatal Intensive Care Units.” Res J Med Med Sci 4, no. 1 (2009): 67–77. DOI: 10.1016/j.jhin.2012.10.017.
Addressing Electricity Insecurity
One study found that only 34% of public hospitals in surveyed sub-Saharan African countries had reliable electricity access [1]. Another more recent study found that over 50,000 health care facilities in sub-Saharan Africa lacked any electricity supply [2].
Our field research found that even facilities with generators experience long daily interruptions of mains electricity. During a 2022 visit to Murtala Muhammad Specialist Hospital in Kano, Nigeria–one of the largest public secondary hospitals in the country–staff explained they experienced long daily interruptions of mains electricity, and that the onsite generator was available only infrequently.
[1] Adair-Rohani, Heather, Karen Zukor, Sophie Bonjour, et al. “Limited Electricity Access in Health Facilities of Sub-Saharan Africa: A Systematic Review of Data on Electricity Access, Sources, and Reliability.” Global Health: Science and Practice 1, no. 2 (2013): 249–61. https://doi.org/10.9745/GHSP-D-13-00037.
[2] Moner-Girona, Magda, Georgia Kakoulaki, Giacomo Falchetta, Daniel J. Weiss, and Nigel Taylor. “Achieving Universal Electrification of Rural Healthcare Facilities in Sub-Saharan Africa with Decentralized Renewable Energy Technologies.” Joule 5, no. 10 (2021): 2687–714. https://doi.org/10.1016/j.joule.2021.09.010.
How to order Otter
Our Vietnamese manufacturing partner MTTS leads all Otter production. MTTS was established in 2004 with the goal of delivering innovative, cost-effective solutions for newborns in need of intensive medical care. MTTS founders Nga Tuyet Trang and Gregory Dajer were recognized by the World Bank and the Schwab Foundation as “Social Entrepreneurs of the Year” in 2017. The Otter Warmer is part of MTTS's comprehensive suite of technologies for neonatal care, which includes a newborn CPAP and warmer. MTTS and their Breath of Life program were featured on PBS Newshour.
DISCLAIMER: The opinions and feedback on the Otter Newborn Warmer referenced on this page were provided by individuals at Murtala Muhammad Specialist Hospital in Kano, Nigeria and Kapiri District Hospital in Zambia, solely for informational purposes. This information is not intended to represent, and should not be construed as, an endorsement, official statement, or approval of the Otter Warmer by the Murtala Muhammad Specialist Hospital or by Kapiri District Hospital. The views shared are those of the contributing individuals and do not necessarily reflect the official position or policy of Murtala Muhammad Specialist Hospital or of Kapiri District Hospital.